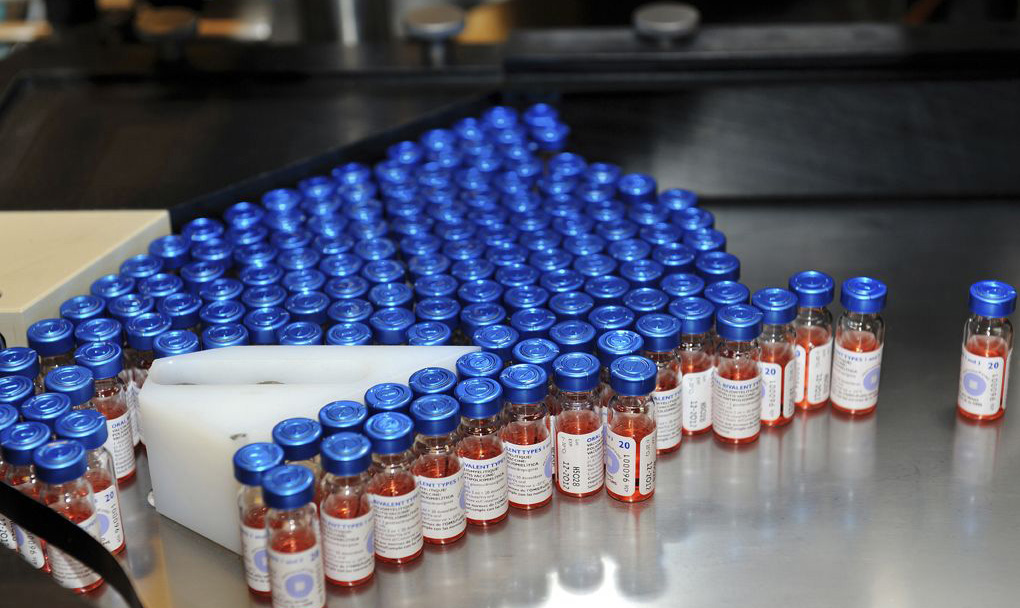
A new technology under development by an academic–industry partnership protects oral vaccines from destruction by the digestive system.
From the mouth to the small intestine, the digestive system presents a series of challenges designed to protect us by killing ingested bacteria. If a microbe survives the digestive enzymes in saliva and the corrosive acid of the stomach, the toxic fat-emulsifying bile acids in the small intestine will probably kill it.
As a first line of defence against disease and infection, the digestive system is an extremely efficient bactericide. However, not all bacteria are pathogenic invaders intent on wreaking havoc. For ‘friendly’ bacteria – such as those used in oral vaccines or as probiotics – keeping them alive long enough to exert their benefits poses a significant challenge to biotechnologists.
Now, a new technology that can safely deliver friendly bacteria to the gut is under development by an academic–industry collaboration as an oral vaccine, and Phase I clinical trials are planned. Developed by Alexander Edwards, Krishnaa Mahbubani and Professor Nigel Slater in the University of Cambridge Department of Chemical Engineering and Biotechnology, the technology has been licensed by biotechnology company Prokarium through Cambridge Enterprise Ltd, the University’s commercialisation arm.
We think this formulation has the potential to be distributed to the four corners of the earth irrespective of supply chain considerations.
Professor Nigel Slater
The oral vaccine is based on inactivated Salmonella enterica serovar Typhi – the pathogen responsible for typhoid fever – which has been engineered to carry proteins from the bacterium that causes traveller’s diarrhoea. When the body makes a strong protective immune response to Salmonella, it does so also to its hitchhiker, making it a powerful vaccine delivery platform for this and potentially any other disease-causing pathogen.
Salmonella is better able to survive the digestive system compared with other microbes and stimulates a strong immune response. This approach also reduces the cost and time of vaccine production, compared with the traditional methods of purifying vaccine proteins from cultured cells.
Mahbubani and Slater particularly wanted to create a vaccine that did not require injection. “Oral vaccines are part of a new generation of needle-free vaccination strategies,” explained Mahbubani. “These strategies are especially suited for use in developing countries, where needle-based vaccination can pose logistical challenges due to the lack of a cold supply chain, hindering the roll out of vaccination programmes.”
Formulating the vaccine for ease of distribution and administration required the production of dried bacteria. However, simply administering dried microbes isn’t the answer. “Protection from saliva can be achieved by swallowing the dried bacteria in the form of a pill or capsule, and the digestive effects of the stomach can be protected against by using an enteric coating that dissolves once the capsule has moved out of the stomach into the more-alkaline small intestine,” said Mahbubani. “In the assault course of the digestive system, the finish line for oral vaccines is the small intestine, where they must survive the detrimental effects of bile. After drying, bacteria lose their natural tolerance to bile. We needed to find a way of stabilising the bacterium in a dried from so that it could be brought back to life before the bile destroys it.”
Once rehydrated, and after the bacterium has reached the lining of the small intestine, it is intercepted by the immune system, eliciting a strong response to the multiplying pathogen. The next time the immune system encounters the same material, usually in the form of the disease-causing pathogen itself, it can react quickly to clear the invader.
The answer to overcoming the encounter with bile came when Edwards made a surprising discovery, as Slater explained: “Drying did not affect the bacteria permanently. On rehydration, they regain their natural protection to bile.
“When we started the project, this wasn’t known. But the finding opened a door to how we could create an oral vaccine that could survive in the digestive system and didn’t require cold storage. We realised that we needed a technology that would allow the bacteria to rehydrate before the bile reaches it.” The solution lay in a novel adaptation of a material called bile-acid adsorbing resins (BARs). Developed in the 1960s to lower cholesterol levels, BARs such as cholestyramine have a long track record of safe oral administration to patients.
The scientists reasoned that if the capsule contained dried bacteria mixed with BAR then, when the enteric coating dissolves and water and bile enter freely, the movement of bile would be held back by the resin long enough for water to rehydrate the bacteria, before the capsule finally breaks open. When she tested the theory, Mahbubani found that this adsorption concept works, even at progressively smaller and smaller capsule sizes.
With funding from the Technology Strategy Board (TSB) and the Biotechnology and Biological Sciences Research Council (BBSRC), the Cambridge scientists have been working with BioPharma Technology Ltd, Microbial Developments Ltd, Cobra Biologics Ltd, and now Prokarium Ltd, as well as Professor Simon Cutting at Royal Holloway College.
Now, as plans are put together for a Phase I clinical trial, work is ongoing to define the precise formulation of bile-adsorbing materials and dried bacterial vaccine, as well as to design the capsule that goes into the trial.
“It’s been very important during the development process that we’ve had the support of the TSB and BBSRC to progress the invention to the stage we’ve now reached,” explained Dr Rocky Cranenburgh, Prokarium’s Chief Scientific Officer. “The combination of BAR technology with the Salmonella vector will allow us to develop an advanced oral delivery platform that gives us the potential to revolutionise vaccinations.
“We are focusing on the development of a dual oral vaccine against typhoid and enterotoxigenic Escherichia coli (ETEC) – a major cause of diarrhoea – for travellers and developing country markets. There are 22 million cases of typhoid every year resulting in 200,000 deaths, so an effective oral vaccine could have a significant impact. Currently there is no dedicated vaccine against ETEC, considered responsible for 300,000–500,000 deaths per year, mostly of young children.”
“This is a great example of the University working with industry, interpreting needs to create a viable product using real science,” added Slater. “We think this formulation has the potential to be distributed to the four corners of the earth irrespective of supply chain considerations.”
This article appears in the latest edition of Research Horizons, the University’s research magazine.
Photo credit: Packaging line by Sanofi Pasteur via Flickr